Chondral Damage
Chondral Damage
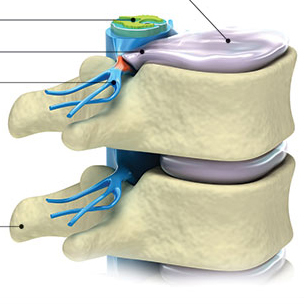
The articular cartilage covers the bony surfaces within the knee joint and is essential for optimal knee function. The articular cartilage in the knee is thicker than in most other parts of the body having to withstand significant loads during daily activities and particularly during high impact activities such as running and jumping sports.
Articular cartilage can be damaged by injury or normal wear and tear, and is often referred to as Condral Damage. Because cartilage does not heal itself well, doctors have developed surgical techniques to stimulate the growth of new cartilage. Restoring articular cartilage can relieve pain and allow better function. Most importantly, it can delay or prevent the onset of arthritis.
Symptoms
The symptoms of an articular cartilage injury are not as obvious as those of a meniscus tear or ligament injury. Symptoms can include:
-
Intermittent swelling - This is often the only symptom, with the loose cartilage fragments floating in the knee causing swelling to occur.
- Pain - Pain can occur with prolonged walking or stair climbing.
- Giving way - The knee may occasionally buckle or “give way” when placing weight on it.
- Locking or catching - The loose, floating pieces of cartilage may block the joint as it bends, causing the knee to lock or catch.
- Noise - The knee may make noise during motion, especially if the cartilage on the back of the kneecap is damaged.
Causes
An articular cartilage injury, or chondral injury, may occur as a result of a pivot or twist on a bent knee, similar to the motion that can cause a meniscus tear. Damage may also be the result of a direct blow to the knee. Chondral injuries may accompany an injury to a ligament, such as the anterior cruciate ligament. Small pieces of the articular cartilage can actually break off and float around in the knee as loose bodies, causing locking, catching, and swelling.
More often, there is no clear history of a single injury. The patient’s condition may result from a series of minor injuries that have occurred over time. Articular cartilage also wears down as we age.
Treatment Options
Articular cartilage degeneration is often treated without surgery. Some measures your SBO orthopaedic surgeon may recommend are:
- Weight loss and changes in physical activity
- Exercises to strengthen the muscles around the joint
- Shock absorbent shoe inserts
- Injections of hyaluronic acid to improve joint lubrication and reduce friction
Your doctor will usually prescribe medications to treat the symptoms and will monitor your progress. Although there are medicines that can treat the symptoms associated with articular cartilage damage, there are no medications that can repair or encourage new growth of cartilage.
Further treatment would require a surgical procedure. The most common surgical treatment involves smoothing the rough areas of the defect with a shaving technique. Factors that influence the choice of procedure include:
- The size and location of the defect in the knee.
- The age and weight of the patient.
- The patient’s future goals and activity level.
- The patient’s motivation and ability to participate in postoperative rehabilitation.
- The patient’s limb alignment: Is the patient bow-legged or knock-kneed?
This arthroscopic technique of shaving, or debridement, has been popular for 20 years and has had very satisfactory results for over 75% of patients. It is a common treatment for patients with a cartilage defect that has not worn all the way down to the bone, especially under the kneecap. This procedure is also used in the more arthritic knee when other resurfacing techniques are not appropriate. Using special arthroscopic instruments, your SBO physician smoothes the shredded or frayed articular cartilage. Ideally, this treatment will decrease friction and irritation, reducing the symptoms of swelling, noise, and pain.
Recovery
The patient’s commitment level to the rehabilitation process is an important factor in determining the outcome of the treatment. Crutch use is minimal and rehabilitation is started immediately after surgery. Regular activities are often resumed within 4-6 weeks.